What Is Scleritis?
What Are the Signs & Symptoms of Scleritis?
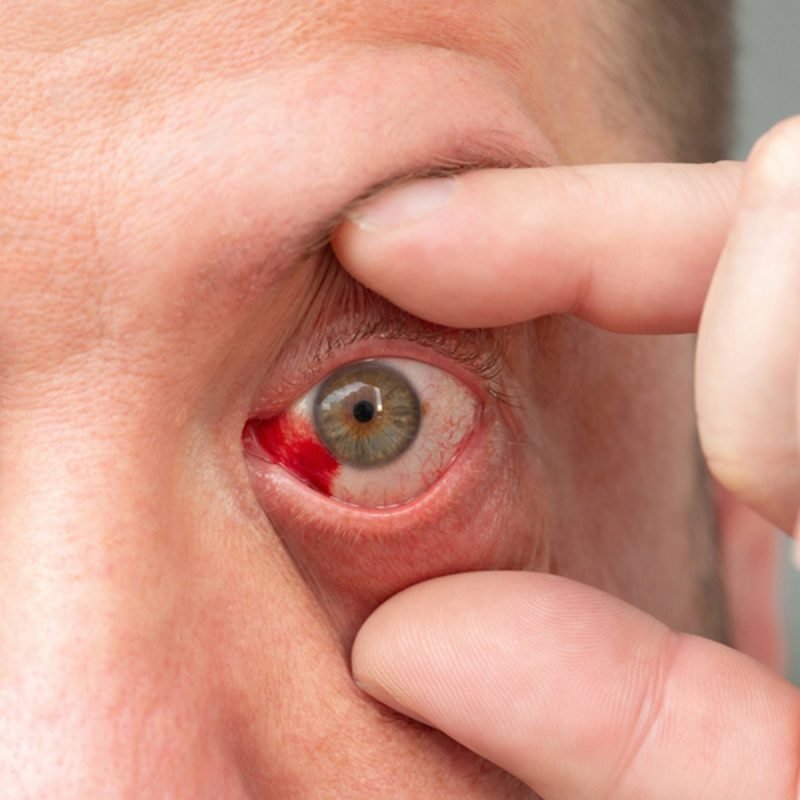
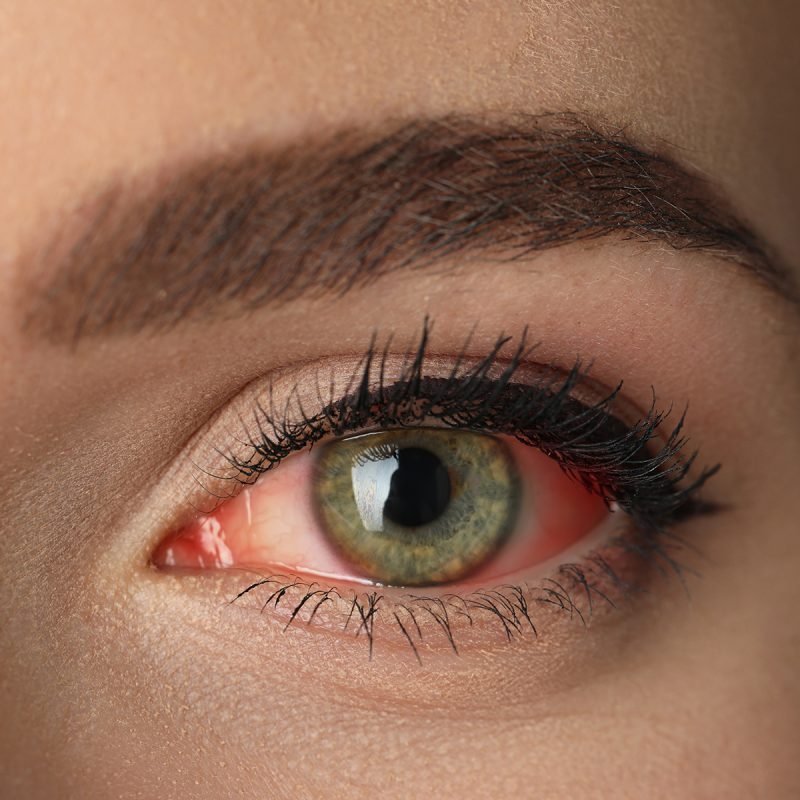
Scleritis causes deep, persistent discomfort and noticeable changes in the appearance of the eye. You may need immediate evaluation if you experience any of the following:
- Intense Eye Redness: The sclera becomes bright red or violaceous, often worsening over time.
- Severe Eye Pain: A deep, penetrating pain that may radiate to the forehead, brow, or jaw — often strong enough to disturb sleep.
- Watering or Excessive Tearing: Persistent tearing without relief, accompanied by irritation or heaviness.
- Light Sensitivity (Photophobia): Bright light becomes uncomfortable, causing squinting or eye strain even indoors.
Dr. Yatri Pandya Bhavsar
MS Ophthalmology, FCORS
Professional Experience
Dr. Nagpal’s Retina Foundation (Shahibaug)
- Cornea Consultant (Morning) — 10:00 am to 2:00 pm
Shivyaa Superspecialty Hospital (Gota)
- Cornea Consultant (Evening) — 02:30 pm to 06:30 pm
Dr. Nagpal’s Centre for Cornea, Navrangpura, Ahmedabad
- Ex - Associate Cornea Consultant
GMERS Medical College & Sola Civil Hospital, Ahmedabad
- Ex - Senior Resident

Different Types of Scleritis
Anterior Scleritis
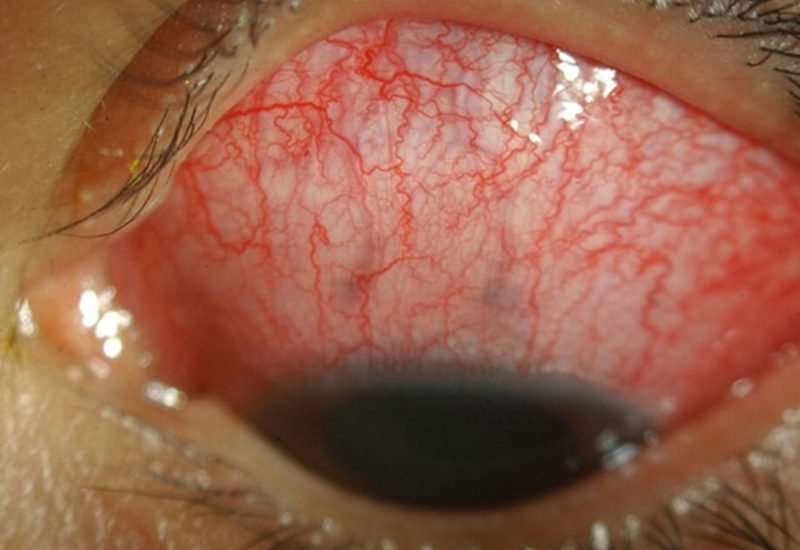
Posterior Scleritis
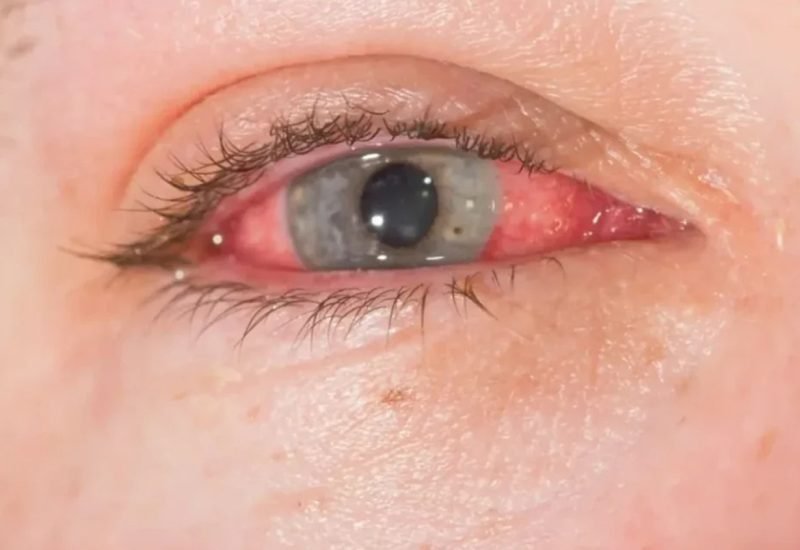
Diffuse Scleritis
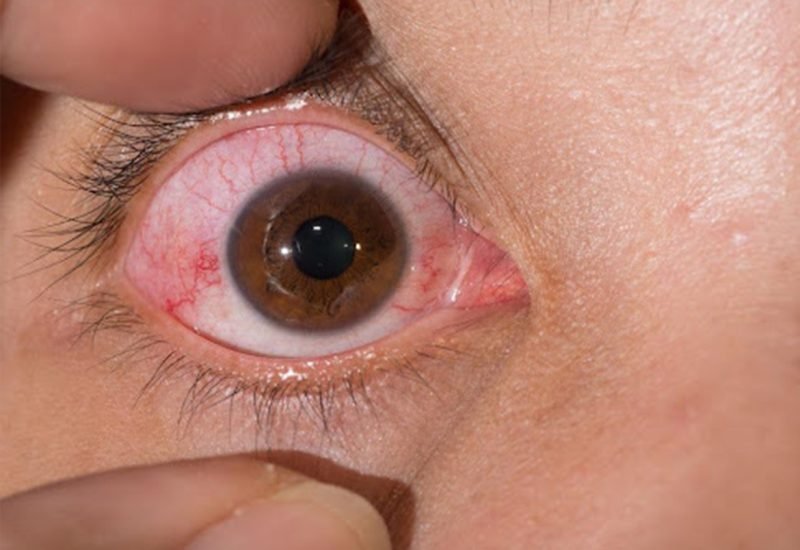
Nodular Scleritis
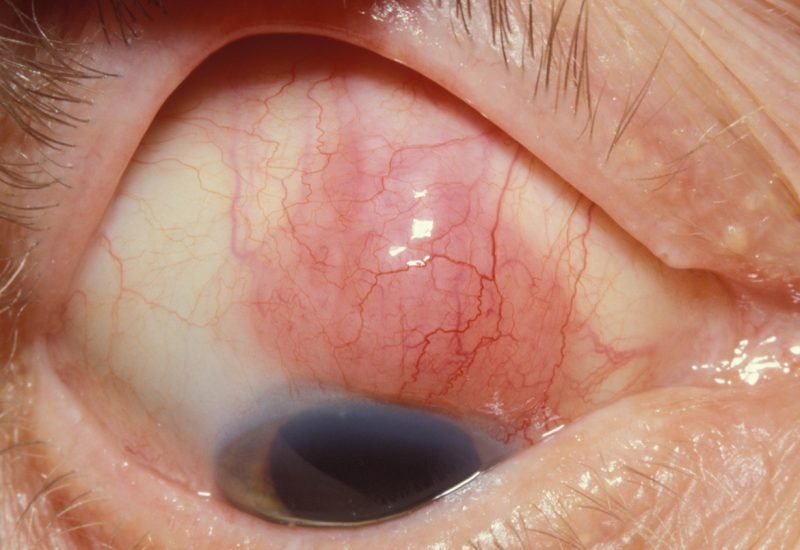
Necrotizing Scleritis
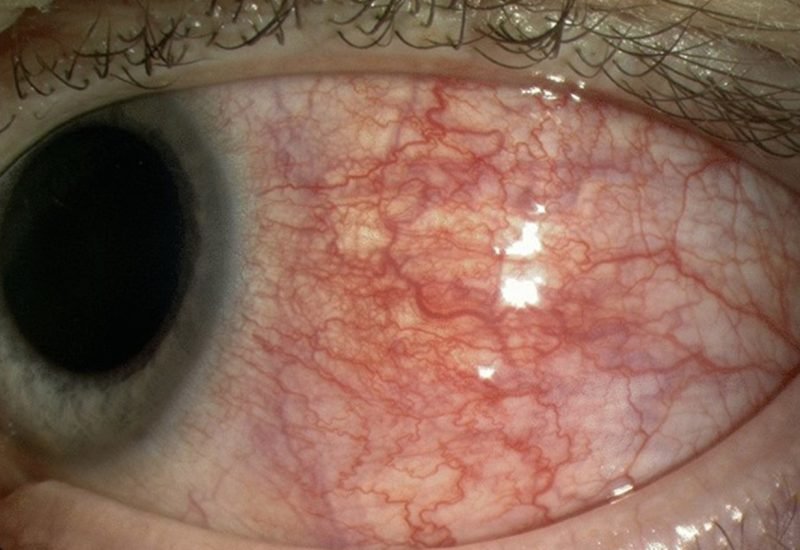
What Causes Scleritis?
Autoimmune Disorders
Autoimmune conditions like arthritis, lupus, Sjögren’s syndrome, scleroderma, and granulomatosis often trigger scleral inflammation, causing persistent pain, redness, and potential tissue damage if untreated.
Systemic Inflammatory Diseases
Chronic inflammatory conditions, including inflammatory bowel disease and connective tissue disorders, can extend immune activity to the eye, leading to deep scleral inflammation and recurrent painful flare-ups.
Infections
Bacterial, viral, and rarely fungal infections may directly inflame the sclera. These infectious causes require prompt treatment to prevent severe complications, structural damage, or progressive vision loss.
Trauma or Injury
Physical injury or post-surgical complications can provoke scleral inflammation. Even minor trauma may trigger significant pain and progressive damage, requiring immediate medical evaluation and prompt management.
Idiopathic Causes
In some individuals, no underlying disease is identified. When the origin remains unknown, scleritis is classified as idiopathic and requires detailed evaluation to monitor progression effectively.
Your Scleritis Care Journey: What to Expect at Shivyaa Hospital
How Scleritis Is Diagnosed
Diagnosing scleritis requires a detailed clinical evaluation supported by advanced imaging. Our goal is to identify the exact type, severity, and underlying cause to ensure timely treatment.
- Comprehensive Eye Examination: Your specialist examines the sclera, cornea, and ocular structures using a slit-lamp microscope to detect inflammation, tenderness, and tissue changes.
- Posterior Scleritis Imaging: If deeper inflammation is suspected, tests such as ocular ultrasound or CT scan help visualize the back portion of the sclera and surrounding tissues.
- Infection Screening: When infection is suspected, a sample of eye discharge may be collected for laboratory testing. Rarely, a biopsy is required for precise diagnosis.
Management & Treatment
Treatment aims to control inflammation, relieve pain, prevent scleral damage, and address any underlying systemic disease contributing to scleritis.
- Anti-Inflammatory Medications: Mild cases may respond to NSAIDs, while most patients require systemic corticosteroids such as prednisone for rapid and effective inflammation control.
- Advanced Steroid Therapy: For recurrent flare-ups or severe inflammation, intravenous corticosteroids may be administered to stabilize the condition quickly.
- Treating Infectious Scleritis: If the cause is bacterial, fungal, or viral, targeted antibiotics, antifungals, or antivirals are prescribed to eliminate the infection and protect the sclera.
- Immunosuppressive Medications: Severe or necrotizing scleritis may require collaboration with a rheumatologist to prescribe medications like methotrexate, mycophenolate, cyclophosphamide, or biologic agents such as rituximab or adalimumab.
- Scleral Patching or Grafts: In advanced cases with tissue thinning or risk of perforation, scleral grafts or patching procedures reinforce weak areas and prevent structural complications.
When to Seek Medical Attention for Eye Problems
01
Severe Pain
02
Vision Loss
03
Redness & Swelling
04
Eye Trauma
Flashes & Floaters
Why Choose Shivyaa Hospital for Expert Care?
Advanced Diagnostic Technologies

Personalized Treatment Plans

24/7 Emergency Services

